Pet surgery by BluePearl.
Precision care for what matters most – helping your pet live a longer and better life.
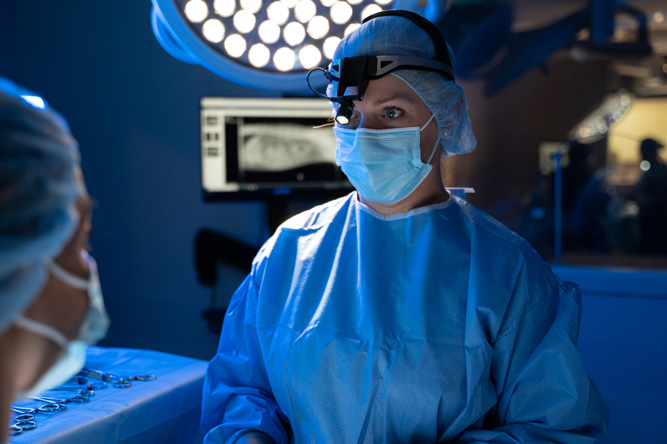
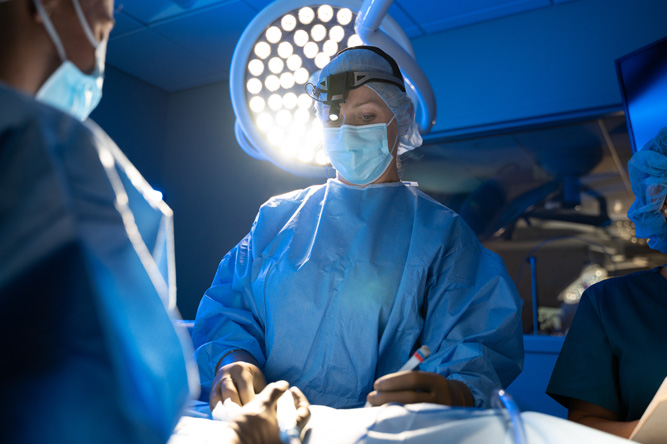
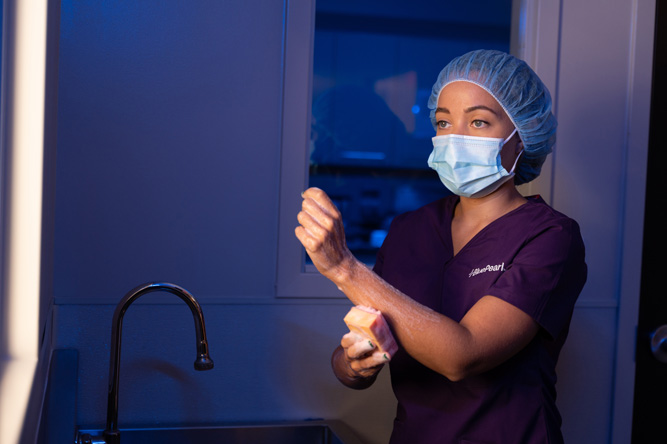
We understand that seeing your pet experience an emergency or condition that requires surgery can be stressful. Fortunately, our veterinary surgery team is made up of experts in performing complex procedures using the latest state-of-the-art techniques and equipment, and we’re here to help.
Our commitment is not just to delivering highly advanced surgical care; it’s to enhance the well-being of your pet and be with you every step of the way.

Conditions we treat.

If your pet has a condition or injury that requires advanced care and procedures, you’ll have an entire surgery team helping to improve your pet’s quality of life so you can get back to what matters most – spending precious moments together.
- Cancer
- Chronic diseases like ear or respiratory tract infections
- Congenital conditions like dysplasia or heart defects
- Emergencies like swallowing a foreign body
- Hernias
- Trauma or injuries, including fractures, ligament and tendon injuries
Services we offer.
Your pet will receive unparalleled medical care during their time at the hospital (and they’ll be spoiled with love and attention, too).
Advanced diagnostics
Your pet can’t tell us what’s wrong, so we use sophisticated diagnostics and imaging tools to uncover the source of the problem.
- Biopsy
- Radiography (x-rays)
- Ultrasound
- CT scan
Treatment plans
Just as no two patients are the same, neither are their treatment plans. Our surgery team has experience with a range of advanced procedures and minimally invasive options to get your pet on the path to wellness, including:
- Orthopedic surgery (for the musculoskeletal system, including bones, joints, ligaments, muscles and tendons)
- Soft tissue surgery (for non-bone tissues and internal organs)
- Minimally-invasive surgery (arthroscopy, laparoscopy, thoracoscopy)
Our board certified specialists and surgery team.
Experience makes all the difference.
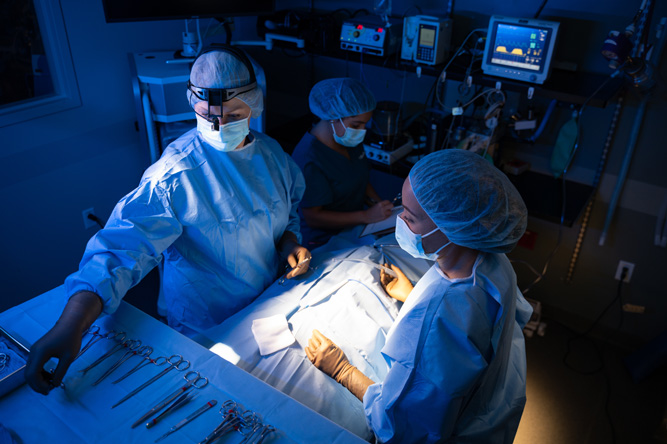
Our surgery team is made up of veterinarians, vet technicians and assistants, and support staff with rigorous training and experience in specialty medicine. The team works hand in hand to provide the comprehensive, compassionate care your pet needs and deserves. Because we’re a multidisciplinary hospital, the team can consult the expertise of other specialty departments, too.
Zachary Kasson
DVMDr. Zachary Kasson is an intern in our surgery service. He finds wound therapy and surgery the most gratifying to perform.
- Internship, Small Animal Medicine & Surgery, BluePearl Specialty + Emergency Pet Hospital, Cary, NC
- Clinical Rotation, North Carolina State University, Raleigh
- Doctor of Veterinary Medicine, Ross University, St. Kitts & Nevis, West Indies
- Bachelor of Science, Integrative Biology, Texas A&M University, Corpus Christi
Dr. Kasson enjoys exploring new places and spending time with his wife and dog.
Meghan Kruse
DVM, DACVS-SADr. Meghan Kruse’s special interests include minimally invasive, urinary and soft tissue surgeries, as well as wound management.
- Diplomate, American College of Veterinary Surgeons-Small Animal
- Residency, Small Animal Surgery, University of Pennsylvania, Philadelphia
- Internship, Small Animal Medicine & Surgery, Michigan State University, East Lansing
- Doctor of Veterinary Medicine, North Carolina State University, Raleigh
- Bachelor of Science, Molecular, Cellular and Developmental Biology, Yale University, New Haven CT
In her free time, Dr. Kruse enjoys spending time with family, repairing small engines, swimming with her local swim team and traveling to new places.
David Lee
DVM, DACVSDr. David Lee is most interested in orthopedic surgery, particularly surgical stabilization of the knee following cranial cruciate ligament rupture and joint replacement.
- Diplomate, American College of Veterinary Surgeons
- Residency, Small Animal Surgery, North Carolina State University, Raleigh
- Residency, Anesthesiology, North Carolina State University, Raleigh
- Internship, Small Animal Medicine & Surgery, Cornell University, Ithaca, NY
- Doctor of Veterinary Medicine, University of Tennessee, Knoxville
- Bachelor of Science, Biology, University of the South, Sewanee, TN
Dr. Lee enjoys woodworking, working about the house and watching his two sons play ultimate frisbee.
Marina Manashirova
DVM, DACVS-SADr. Marina Manashirova’s interests include surgical oncology, wound management, and any condition involving the thorax.
- Diplomate, American College of Veterinary Surgeons-Small Animal
- Residency, Small Animal Surgery, University of Illinois, Urbana-Champaign
- Internship, Small Animal Surgery, Gulf Coast Veterinary Specialists, Houston, TX
- Internship, Small Animal Medicine & Surgery, Purdue University, West Lafayette, IN
- Doctor of Veterinary Medicine, University of Tennessee, Knoxville
- Bachelor of Science, Biology, Misericordia University, Dallas, PA
Dr. Manashirova’s family consists of her husband, daughter, and a 24-year-old ball python. She enjoys hiking, kayaking, and spending time with family and friends.
What to expect.
We want you to be prepared for your pet’s visit to the surgeon, so you have one less thing to worry about. Our entire BluePearl team will be with you every step of the way.
Before your visit
- Make a consultation appointment by calling us directly or via referral from your pet’s primary vet.
- We’ll get records from your primary or emergency vet before your visit and collaborate with them to discuss your pet’s history and current condition.
During your visit
- When possible, we’ll examine your pet with you by their side to make them more comfortable. If additional tests are needed, we’ll discuss those options with you.
- You’ll have plenty of time and opportunity to ask questions as we go over your pet’s diagnosis and treatment plan options together.
- If appropriate, we’ll schedule your pet’s procedure and make sure you’re aware of any symptoms you should watch out for at home.
After your visit
- Our team will continue to partner with your primary veterinarian as part of the ongoing management of your pet’s care.
- You know your pet better than anyone, and you play a crucial role in their treatment plan. If you have any concerns about providing care at home (such as giving medication, maintaining a specific diet or monitoring your pet’s symptoms), let us know – we’re here for you.