Anesthetic-induced hypothermia is very common in veterinary patients.
Unfortunately, the incidence of anesthetic-induced secondary hypothermia in small animal patients has remained relatively consistent throughout the past 30 years.
In 1973, the incidence was reported as 100% by Evans et al., and it was reported to be 97.4% by Redondo et al. in 2012. Normal core body temperature in dogs ranges from 100-102.50F, and awake patients can regulate their core body temperature within 0.20C of normal.
Mild secondary hypothermia is defined as 98-99.90F; moderate hypothermia is 96-980F; severe hypothermia is defined as 92-960F; and critical hypothermia is <920F. There are three phases of anesthetic-induced hypothermia.
During phase 1, the initial core body temperature decreases rapidly by 1-50C. This is the most rapid decrease.
During phase 2, which occurs over the following 2-3 hours, the temperature decreases slower.
Phase 3 is essentially the plateau temperature phase.
How it Happens
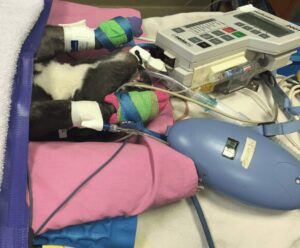
The degree to which general anesthesia will cause hypothermia is dependent upon a number of factors, including the pre-anesthetic peripheral body temperature, body condition, severity of disease, and surface area of the patient.
Surface area plays a large role in cutaneous heat loss. With a larger exposed surface area, there will be increased conduction of body heat into the environment.
Small dogs, cats, neonates and animals in thin body conditions have a greater surface area to body mass ratio, thus making them much more susceptible to rapid heat loss and less efficient with compensatory heat production.
Fat, serving as an effective insulator, conducts only about one-third as readily as other tissues, thus slowing the transfer of body heat to the environment.
Effects
Numerous adverse effects secondary to anesthetic-induced hypothermia have been documented in human and veterinary medicine. Kurz et al. showed that a 1.90C drop in temperature tripled the incidence of surgical wound infection.
Pottie et al. demonstrated a direct and significant correlation between hypothermia and prolonged recovery rates.
Beal et al. found that for every additional hour under anesthesia there was a 30% increased risk for post-operative wound infections. Other notable effects of anesthetic-induced hypothermia include prolonged hospitalization and subsequent increased cost to owners.
Standard Warming Methods
Passive surface, active surface, and active core are the basic types of warming methods. Surgical drapes, cotton blankets, bubble wrap, and plastic sheeting are types of traditional passive surface methods. Warming panels, circulating water blankets, and forced-air delivery systems are types of active surface methods. Warmed, incubated intravenous fluids and IV fluid warmers are examples of active core warming modalities.
Fluid Line Warmers
In a survey of 150 general veterinary practices by Dix et al., 98.7% used warmed IV fluids and blankets. No hospitals used IV fluid warmers or other external forced heating systems. Unfortunately, since the publication of the Dix et al. study, the use of pre-warmed intravenous fluids has been proven ineffective in a randomized in-vitro fluid trial.
In this study by Soto, Towle Millard et al., IV fluid was tested at five temperatures in five-degree increments. The tested fluid range was 1040F to 140oF (400C to 600C). Each of the five temperatures were tested at nine different fluid rates, ranging from 10 to 300 ml/hr.
Fluids up to 1400F have been demonstrated to cause minimal complications in both laboratory canine testing and human combat situations that have required medical care in hot climates. Fluid temperatures were not tested above 1400F because medical grade plastics and adhesives typically melt around 1580F. All fluid temperatures were less than room temperature fluids, except at 300 ml/hr.
Fluid line warmers are a different type of active core warming. In phase 1 of a study by Lee, Towle Millard et al., distance-dependent and distant-independent devices were tested. Surprisingly, distant-dependent proved to be the more effective device.
In phase 2, two distant-dependent devices were then tested, and the more cost effective, i-Warm device, proved to be superior. Not surprisingly, faster fluid rates and closer connection of the device to the intravenous catheter resulted in higher output temperatures.
Our Procedure in Kansas City
In our surgical service, we use a combination of passive surface, active core, and active surface modalities. Our team of skilled nurses perform an expeditious patient preparation. If, however, the patient preparation is arduous such as for large skin and reconstructive surgeries, then we place baby booties on paws; patients are on circulating warming pads; and IV fluid warmers are used while the patient is in the preparatory room.
Once the patient is transferred into the operating room, we continue to use baby booties on the paws, circulating warm water blankets, forced air heating systems such as a Bair Huggerä (recommend to turn on once all surgical drapes and clamps are established) and/or a HotDogâ device followed by blankets and the surgical drapes. (Note: The Hot Dog device manufacturer does not recommend its use in the presence of flammable anesthetics or oxygen-enriched environments.)
Even with complicated and prolonged anesthesia and surgical cases of 2-3 hours, our patients typically will come out of the operating room with a temperature above 99.50F when extubated.
Conclusion
Although anesthetic-induced hypothermia is a common complication of veterinary surgery, BluePearl surgeons and vets use advanced monitoring and considerations to ensure patients are safe while undergoing surgery. Talk to your vet about a referral to one of our BluePearl Pet Hospitals near you if your pet needs surgery or needs anesthesia for a diagnostic test.