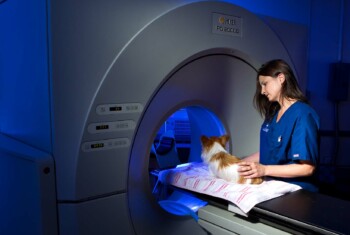
Feline hyperthyroidism: Causes, symptoms, treatments.
Feline hyperthyroidism was an unknown entity until 1978 when Dr. Jean Holzworth at Angell Memorial Animal  Hospital in Boston first diagnosed it. In 1979, Dr. Mark Peterson, who had also recognized the disease at the Animal Medical Center in New York, gave the first lecture presentation on the disease.
Hospital in Boston first diagnosed it. In 1979, Dr. Mark Peterson, who had also recognized the disease at the Animal Medical Center in New York, gave the first lecture presentation on the disease.
Initial cases were cats that had extreme weight loss in the face of a voracious appetite. Initial treatment was with thyroidectomy, later followed by medical therapy with PTU, which gave way to Methimazole. Shortly thereafter in 1981, Dr. Peterson used I-131 for the first time to treat a cat with hyperthyroidism. In 2011, Hills released Y/D, which is a diet extremely restricted in iodine concentration for the treatment of feline hyperthyroidism.
Today hyperthyroidism is the most frequent endocrine disease in cats and is reported to occur in 10% of cats older than ten years of age. It is primarily reported in cats between four and 22 years of age, with fewer than 5% of cases occurring in cats younger than eight years of age.
Since T4 has been included in most feline panels, the disease is recognized earlier in its course before cats become debilitated. Most cases are due to adenomatous hyperplasia or thyroid adenomas, with both lobes being affected in 70% of the cases. Ectopic hyperthyroid tissue is noted in 4.8% of cases. Fortunately, thyroid carcinomas are seen in less than 2% of the cases.
Possible causes.
The actual cause of hyperthyroidism is unknown but is thought to be secondary to a circulating substance, since both lobes are most commonly affected, and there is no physical connection between them. Possible causes that have been speculated include:
- Dietary factors: Canned cat foods were first introduced in the 1960s, with initial introduction on the east and west coasts, the areas where the disease was first noted in the 1970s. Cats eating mostly canned foods, especially canned fish, are at a higher risk.
- Signaling agents: Cats with thyroid adenomatous hyperplasia have decreased levels of G protein in their thyroids, which may decrease cAMP inhibition of cell growth. The oncogene C-Ras has been found in cats with adenomatous hyperplasia and thyroid adenomas.
- Environmental exposure: Cats with hyperthyroidism have demonstrated increased serum levels of polybrominated diphenyl esters (PBDE) ꟷ which are flame retardants ꟷ in several studies, and there is evidence that exposure to cat litter may increase the risk of hyperthyroidism. Negative associations have also been demonstrated: 1. Siamese and Himalayan breeds are at decreased risk for hyperthyroidism, and no risk has been associated with the use of flea products.
Signs and symptoms.
Common clinical signs associated with hyperthyroidism include weight loss, polyphagia, polydipsia, polyuria, vomiting, diarrhea, weakness, hyperactivity, irritability and aggression, while 10% of affected cats demonstrate lethargy, anorexia and mental dullness (so-called apathetic hyperthyroidism).
Physical exam findings include a palpable thyroid nodule in 80% of cases, muscle atrophy, poor hair coat, overgrown nails, tachycardia and systolic heart murmurs. Hypertension is found in 15 – 20% of cases, and heart failure is seen in approximately 2% of hyperthyroid cats.
Laboratory results associated with hyperthyroidism may include mild polycythemia, a stress leukogram, elevations of ALKP, ALT and AST in 90% of cases and azotemia in 20%. Creatinine levels may be decreased secondary to muscle atrophy.
Thoracic radiographs demonstrate cardiomegaly in 20-30% of cases, although with concentric hypertrophy may not manifest as cardiomegaly. Radiographic evidence of heart failure is seen in fewer than 5% of cases.
Diagnosing the condition.
The diagnosis is based on the concurrent findings of appropriate clinical signs, a possible palpable thyroid nodule and serum thyroid testing. The vast majority of cats with hyperthyroidism (90%) have an elevated total T4 based on  equilibrium dialysis. Since T4 levels can fluctuate, a cat with suspected hyperthyroidism (based on clinical signs and/or a thyroid nodule) and a normal T4 should be retested another day.
equilibrium dialysis. Since T4 levels can fluctuate, a cat with suspected hyperthyroidism (based on clinical signs and/or a thyroid nodule) and a normal T4 should be retested another day.
As cats age, T4 levels in cats without hyperthyroidism tend to decrease into the low normal range. In a cat with clinical signs of hyperthyroidism and a high normal T4 level, then a free T4 (FT4) is indicated to further define the diagnosis. A FT4 has a high sensitivity but less sensitivity than a T4, so it should not be relied upon as a sole diagnostic test for the diagnosis of hyperthyroidism in the absence of clinical signs, a palpable nodule or a high resting T4.
Treatment options.
Therapeutic options for hyperthyroidism include:
- Methimazole
- Surgery
- Y/D diet
- I-131 therapy. The goal of therapy is to reduce the T4 level to 1.5 – 2.5 ug/dl.
Methimazole.
Methimazole is usually used as the first-line treatment. It can be used to stabilize a hyperthyroid cat prior to surgery, as an ongoing therapy or to evaluate the response of renal function to control of hyperthyroidism. Treatment is usually initiated at a dose of 2.5 mg per cat twice daily. It can be administered orally or transdermally. Adverse effects with Methimazole are seen approximately 20% of the time (usually during the first three months of therapy) and include anorexia, vomiting, lethargy, diarrhea, leukopenia, lymphocytosis and eosinophilia.
In less than 5% of cases, severe neutropenias and thrombocytopenia can be seen. Heptopathy and facial pruritus (especially around the base of the ears) can also be seen. Hematology, chemistries, urinalysis and T4 levels should be checked every 2- 4 weeks initially and then less frequently as control is achieved. It is recommended that the T4 level be tested six hours post pill. One additional concern with the use of Methimazole is that it only blocks T4 synthesis but not growth of the abnormal thyroid tissue, therefore the dose will probably need to be increased over time.
This is especially a concern in cats diagnosed at a younger age. It is the recommended therapy for cats with poor renal function, as the dose can be titrated to achieve a balance between renal function and hyperthyroidism.
Surgery and diet.
Surgery is the original approach to therapy. If it is pursued, pretreatment with Methimazole to decrease the risk of complications is recommended. Since the disease usually involves both lobes, bilateral thyroidectomy is recommended. Potential complications include Horner’s syndrome, voice change, laryngeal paralysis, hypoparathyroidism and hypothyroidism. Due to the potential for hypoparathyroidism, it is recommended that iCa be checked beginning three days post operatively. If hypocalcemia develops, it should be treated with Calcitriol and Ca supplementation. It frequently resolves within several months.
Hills Y/D diet.
 The Hills Y/D diet is an extremely restricted iodine diet that results in cats being fed it exclusively become euthyroid. Exposure to other sources of iodine, including other foods, food bowls that have contained other foods, treats, well water, prey or human food will negate the effect of Y/D diet. It is also reported that the T4 tends to be in the high normal range in cats fed this diet. As with Methimazole, Y/D does not prevent enlargement of the thyroid.
The Hills Y/D diet is an extremely restricted iodine diet that results in cats being fed it exclusively become euthyroid. Exposure to other sources of iodine, including other foods, food bowls that have contained other foods, treats, well water, prey or human food will negate the effect of Y/D diet. It is also reported that the T4 tends to be in the high normal range in cats fed this diet. As with Methimazole, Y/D does not prevent enlargement of the thyroid.
Radioactive iodine treatment (I-131).
Radioactive iodine (I-131) can cure hyperthyroidism 95% of the time with a single dose. It is taken up by the overactive thyroid cells, killing them and nearby cells as its radiation is given off over a very short distance. 2.5% of treated cats become hypothyroid and they may require thyroid supplementation. The other 2.5% remain hyperthyroid and frequently can be controlled with a second dose of I-131.
I-131 is the favored therapy by many, especially in younger cats, as it can destroy the abnormal thyroid tissue and can treat the rare thyroid carcinoma. I-131 obviously involves the use of a radioactive compound, which is a concern for human exposure.
Once a cat is treated, it must remain in the hospital until its radiation level is low enough for safe discharge, as determined by state or federal regulation. Depending on the dose administered and the locale, the cat will need to be hospitalized for 5 – 14 days. Once discharged, there are also handling restrictions at home. Most of the emitted radiation stays with the cat, however some is excreted in the saliva and urine.
For the first two weeks following discharge:
- The owners may not have close contact with the cat (defined as holding it) for more than 15 minutes per day and they must wash their hands afterward.
- The cat cannot go outside.
- The cat cannot be around women who are pregnant, women who are trying to become pregnant or children under 12 years of age.
- The cat cannot sleep with the owner.
- The litter box must be lined with plastic liners; the owner must wear gloves when cleaning it and wash their hands afterward. The litter may be disposed of normally. After this two-week period, all activities can return to normal.