Increased legalization.
As of November 2020, a total of fifteen states have legalized recreational marijuana use. This has created an environment within the homes of many owners wherein their pets are increasingly exposed to varying forms of tetrahydrocannabinol or THC, posing serious health implications.
The most recent available nationwide statistics saw a 765% increase in case calls from 2018 to 2019 for ASPCA’s Poison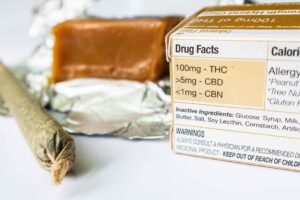 Control and a 448% increase over 6 years for Pet Poison Helpline. We can reasonably assume this to be an underrepresentation if we consider that some owners never report to any toxicology service or that many suspect cases are never confirmed via owner or veterinarian callbacks to these lines; additionally, there are veterinarians who never seek assistance with treating these cases.
Control and a 448% increase over 6 years for Pet Poison Helpline. We can reasonably assume this to be an underrepresentation if we consider that some owners never report to any toxicology service or that many suspect cases are never confirmed via owner or veterinarian callbacks to these lines; additionally, there are veterinarians who never seek assistance with treating these cases.
Knowing this, we can reasonably expect to see a continued increase in the number of marijuana ingestion cases within the hospital, making it vitally important that all veterinary professionals, front and back of house, understand how to recognize the clinical signs of marijuana toxicity and address the subject with owners while remembering that our first priority is making sure the pet is treated appropriately.
The cause.
 Delta-9-tetrahydrocannabinol is the key molecule in marijuana that causes toxicosis in dogs, and occasionally cats, by reacting with cannabinoid receptors in the brain. These receptors release acetylcholine, serotonin, norepinephrine, gamma-aminobutyric acid, and dopamine that cause the clinical signs. THC is rapidly absorbed through both oral ingestion and inhalation, and onset of clinical signs can be as quick as 5 minutes, but usually manifest around 30 minutes after exposure and lasting up to 3 days. The most common clinical signs seen are ataxia, hyperesthesia, hypoventilation, tachy- or bradycardia, hypoventilation, hypothermia, urinary incontinence, and ptyalism.
Delta-9-tetrahydrocannabinol is the key molecule in marijuana that causes toxicosis in dogs, and occasionally cats, by reacting with cannabinoid receptors in the brain. These receptors release acetylcholine, serotonin, norepinephrine, gamma-aminobutyric acid, and dopamine that cause the clinical signs. THC is rapidly absorbed through both oral ingestion and inhalation, and onset of clinical signs can be as quick as 5 minutes, but usually manifest around 30 minutes after exposure and lasting up to 3 days. The most common clinical signs seen are ataxia, hyperesthesia, hypoventilation, tachy- or bradycardia, hypoventilation, hypothermia, urinary incontinence, and ptyalism.
For many technicians, the key signs during triage that frequently prompt suspicion of ingestion are hyperesthesia, commonly described by owners as restlessness or agitation and urinary incontinence. Though rare, coma and even death are possible, so treatment should commence as quickly as possible.
Treatment.
Treatment of marijuana toxicity is largely supportive and can occur on an inpatient or outpatient basis depending on case severity. For all hospitalized patients, treatment should include IV fluid diuresis with crystalloids generally given at 1.5 to 2 times maintenance rate, GI support with antacids and antiemetics, and management of neurologic signs with  anticonvulsants and anxiolytics when necessary.
anticonvulsants and anxiolytics when necessary.
THC is a lipophilic molecule; therefore oral administration of activated charcoal can help reduce the occurrence of enterohepatic recirculation. In the same manner, more severe cases can benefit from the use of lipid therapy.
Intralipids, administered intravenously, bind with the THC molecule and reduce the availability for absorption within the bloodstream. Plumb’s recommends starting lipid therapy with a 1-minute IV bolus of 1.5-4ml/kg, followed by 15ml/kg/hr CRI for 30-60 minutes, and additional slow boluses of 7ml/kg, as needed until a response to treatment is noted. (Plumb’s) When administering IV lipid therapy, it is critical to monitor plasma for lipemia, in an effort to prevent secondary disease such as pancreatitis; this can be performed easily by spinning down a hematocrit tube.
Monitoring.
Monitoring of the hospitalized patient includes hourly respiratory and seizure watches, telemetry, and vital signs and serial blood pressures. It is important to factor in appropriate treatment and monitoring for additional toxin exposure, such as chocolate, xylitol, or raisins, as most marijuana ingestion occurs due to consumption of edibles that may contain these ingredients. For milder cases in which the owner elects outpatient therapy, patients are generally given subcutaneous fluids, IV or subcutaneous antiemetics, and an oral dose of activated charcoal, then discharged contingent that the owners monitor their pet closely for changes and return immediately if clinical signs do not improve. In general, hospitalized patients are discharged upon resolution of clinical signs.
A reminder.
The most important thing to remember when triaging and treating cases of marijuana ingestion is to withhold assumptions and judgement of the client. Even with legalization, many clients are still very reluctant to admit possession for fear of repercussions. Though we are legally and ethically required to report suspected cases of animal abuse and neglect, the vast majority of marijuana ingestion cases are incidental, and the number-one priority should always be treating the patient.