What are seizures?
Seizures in dogs are one of the most common neurologic conditions found in the species. They are usually characterized by repetitive motor activity of a part of the body (focal) or the entire body (generalized), secondary to abnormal electrical activity inside the brain.
Depending on the underlying cause, multiple options for medical treatment exist, and many dogs can live a long, happy life with this diagnosis.
Clinical signs and symptoms of seizures
Seizures are often confused with other types of involuntary activity, including tremors, acute vestibular conditions (vertigo), syncope (cardiac/fainting) episodes or even dreaming. Your veterinarian will ask detailed questions regarding the timing and nature of the event. It can be very helpful to take a video of your dog’s suspected seizure activity and show it to your veterinarian.
During a seizure, dogs may lose consciousness, have involuntary rigidity followed by paddling (tonic-clonic convulsions), lose control of the bladder or bowels, or have altered perceptions of their surroundings (visual or auditory hallucinations).
In some instances, dogs may remain awake and alert and exhibit focal twitching or fly-biting. In rare cases, abrupt behavioral changes such as tail-chasing or periods of fear or rage may also be classified as seizures.
Causes
In general, seizures always indicate abnormal forebrain electrical activity. Depending on your dog’s age, vaccination status, breed, history and even geographic location, some causes will be more likely than others.
In young dogs, infectious diseases, congenital problems, low blood sugar or toxicities are more common causes.
In older dogs, autoimmune/inflammatory conditions, brain tumors or vascular events are more common causes.
And, in many dogs between six months and six years, idiopathic epilepsy (without an underlying cause) is the most common diagnosis. It’s important to remember that idiopathic epilepsy is a diagnosis of exclusion, which requires ruling out other causes using a combination of lab work, advanced brain imaging and spinal tap.
Getting a diagnosis
Your primary or emergency veterinarian may order diagnostic tests to screen for certain conditions. However, a referral to a veterinary neurologist (available in many BluePearl hospitals) can provide an even more comprehensive evaluation of your dog’s seizure disorder.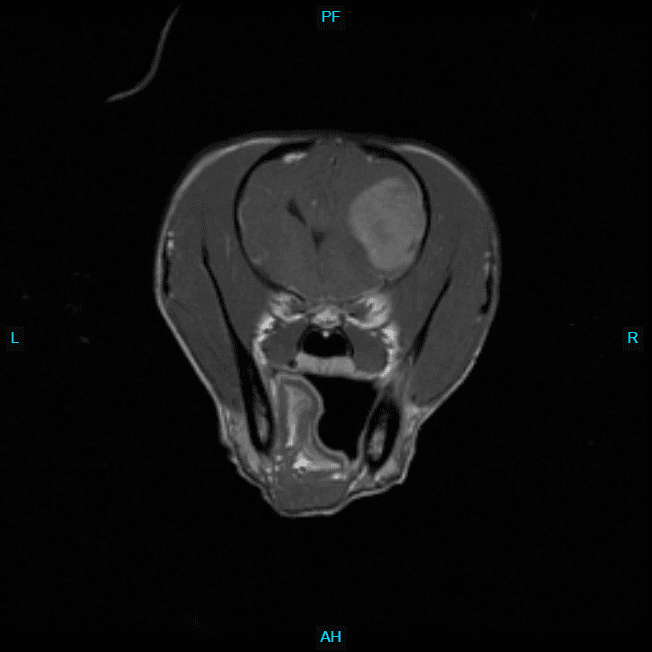
A veterinary neurologist will perform a full neurologic examination at the time of the appointment and may recommend more specific testing, such as:
- Chest x-rays or abdominal ultrasound to screen for diseases such as tumor metastasis
- Liver function testing to evaluate for congenital liver conditions (liver shunts)
- Infectious disease testing (serology or PCR) relevant to the geographic area
- Toxicology screening for heavy metals
- Brain imaging (MRI, CT, etc.), which is performed under general anesthesia to evaluate brain anatomy and structural changes
- Spinal tap to look for evidence of inflammation, infection or malignancy
Questions for your doctor
When consulting with your pet’s veterinarian, consider asking questions like:
- What are the benefits and side effects of the different medication options for my dog?
- How could a veterinary neurologist help with the diagnosis and long-term management of my dog?
- How comfortable are you managing a complex seizure case if multiple medications become necessary?
- Should I get a referral to a veterinary neurologist before a second medication is added?
Treatment
If an underlying condition is identified as the cause for seizures, treatment should be aimed at that condition; only sometimes is separate seizure management needed. In many cases, an underlying condition is not identified, and long-term anti-epileptic medications are recommended.
In 2015, the American College of Veterinary Internal Medicine published consensus guidelines on seizure management in dogs. Treatment is recommended in dogs that meet the following criteria:
- Identifiable structural lesion (tumor, etc.) or prior history of brain disease or injury
- Seizures lasting more than five minutes, or three or more generalized seizures within a 24-hour period
- Two or more seizure events within a six-month period
- Prolonged, severe or unusual postictal (post-seizure) periods
Several options for treatment exist, all requiring daily administration of oral medications. Because compliance is one of the keys to treatment success, it is particularly important that you and your prescribing veterinarian are on the same page about reliable administration, medication costs, follow-up lab work and the pros and cons of each available medication. What may be right for one owner and dog may differ from what’s right for another.
It’s ideal to reach a seizure frequency of at least six weeks or longer. Some animals can go for months or years without seizures, while others may require multiple agents for optimal control. Unfortunately, certain breeds can be particularly challenging to control, such as German shepherds, huskies, Saint Bernards and Australian shepherds.
Seizures can be a medical emergency, and it’s critical to understand when to seek emergency care for your dog. If your pet experiences any of the following, contact your veterinarian or local emergency clinic for guidance:
- Multiple seizures with incomplete recovery in between. This is called status epilepticus. Untreated status epilepticus can result in permanent brain damage, hypoxia, overheating and brain swelling.
- Multiple seizures with short periods of normalcy in between. This is called cluster seizures. This can then progress to status epilepticus.
- Trouble breathing after a seizure, as this may indicate lung edema and require oxygen support.
- A prolonged post-seizure (postictal) period.
- Ingesting a substance that can cause seizures. An emergency veterinarian may contact a toxicologist and be able to provide specific treatment if one is available.
- Low blood sugar in puppies. Place a small amount of sugar water or Karo syrup on the gums and seek veterinary care as soon as possible.
BluePearl’s emergency doctors commonly manage seizures and can evaluate your dog to provide a number of short and long-term treatment options to best suit you and your dog’s needs. In some instances, an emergency doctor may recommend that your dog be hospitalized for 24 hours on a continuous infusion of a medication to stop seizure activity and start a long-term anti-epileptic medication.
Prevention
If your dog is on seizure medication, it is imperative to administer it on time and to recheck blood levels as recommended. Some medications, like levetiracetam, will not be effective if not administered every eight hours (or every 12 hours, for the extended-release option). Others, like phenobarbital, require monitoring of lab work values and drug levels to ensure normal metabolism.
A good idea is to keep a “seizure diary” for your pet to track seizure frequency, duration, time of day and medications your pet is taking. This log can help your veterinarian adjust treatments and monitor progress.
Lastly, if your dog is prone to cluster seizures, your veterinarian may prescribe a short course of additional benzodiazepines to have on hand at home to break a cluster and prevent hospitalization.
Prognosis
As with many diseases, realistic expectations and open communication are key to managing seizures. The family, primary veterinarian, local emergency clinic and veterinary neurology specialist are all part of the healthcare team and should seek to work together to provide the best outcomes.
In many dogs, seizures require life-long management, but many dogs can live full and happy lives with this condition. If you think your dog’s seizures may be linked to being exposed to a toxin, or head injury, it’s important to seek the care of an emergency veterinarian immediately. Your emergency vet will most likely refer your dog to a veterinary neurologist to follow up on diagnosis and long-term treatment if it is determined your dog’s seizures are caused by an illness.
BluePearl Pet Hospitals provide both emergency and specialty neurology services in many of our hospitals around the country. Find a BluePearl veterinarian to get your dog treatment for seizures.