3D printing in veterinary orthopedics offers new treatment options.
Angular limb deformities, whether congenital, developmental or traumatic in origin, can be challenging to treat. Even with advanced imaging, it can be hard to visualize the anatomy and anticipate the most appropriate solution for a given abnormality. It is now conveniently and economically possible to convert computed tomography (CT) scan DICOM image data into formats that are more easily and intuitively interpreted.
There are many software solutions available that can create a multiplanar reconstruction for visualization on a computer screen. It has also recently become possible to reproduce three-dimensional models of a patient’s individual anatomy, which can be manipulated for the purposes of surgical practice and planning.
This article’s purpose is to summarize the process, using the example of a distal femoral varus deformity that presented recently for surgical management.

3D-printed model of the deformed femur showing supports to enhance stability during printing.
A CT scan was performed on the patient’s pelvic limbs, and the DICOM files were stored on our hospital’s image server. This data was downloaded and imported into a program called “3Dslicer” for conversion into an anonymized NRRD file format, selecting the region of most interest. This file was then uploaded for conversion by an online program called “democratiz3d” into a 3D-printable version known as an STL file. This generated a smooth-surfaced model that could be visualized in any orientation on a computer screen.
A 3D printer-specific program named Cura was then used to create a gcode file, including parameters such as the type of printer filament, orientation of the object to be printed, temperature of the extruder, and the addition of supports to stabilize the model during the print process. The entire process for this life-sized femur was accomplished in a few hours.
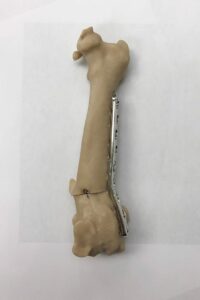
Pre-operative simulation of the corrective osteotomy.
It was then possible to measure the appropriate amount of correction for the angular deformity by manipulation of the reconstructed image on the computer screen, and simulate a corrective osteotomy preoperatively using the printed 3D model. This also allowed the contouring and application of an appropriately sized implant to the printed plastic model. The pre-contoured implant could then be sterilized for use during the actual surgical procedure.
There are also companies that are able to fabricate custom orthopedic implants based on similar scan data, but the process described above allows the utilization of standard implants in a more efficient fashion, by eliminating much of the time required for implant selection and contouring intra-operatively, which can often involve a lot of trial and error. When implant inventory is not unlimited, achieving the appropriate result initially can be very helpful to the patient and surgeon.
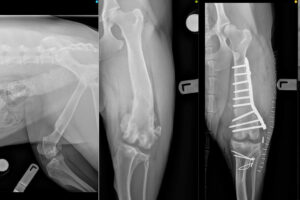
Pre- and post-operative radiographs, courtesy of Dr. Ralph Mallard.
There are printer-specific limitations regarding the size of model that can be accommodated, as well as the type of material that can be printed. Polylactic acid (PLA), ABS, and nylon are commonly used plastics in 3D printing with varying degrees of strength, flexibility and heat resistance. It is possible to gas sterilize models for intra-operative reference, and individualized 3D-printed drill guides have been fabricated for safer intra-operative placement of spinal implants.
Since my original publication describing 3D surgical procedure simulation of pelvic osteotomies for the treatment of hip dysplasia in 1996, the advances in technology have been astounding. Gone are the days of storing CT data on large reel-to-reel magnetic tapes. The potential applications of this technology are seemingly endless and limited primarily by the imagination and resourcefulness of the clinical team. The potential educational and promotional benefits are intriguing as well.