Diagnosing and Treating Spinal Cord Injuries
The spinal column is subject to fractures, luxations and subluxations as a result of major traumatic injuries. Ten percent of dogs suffering blunt trauma sustain vertebral column injuries, with approximately half of these injuries being due to vehicular trauma.
Other causes of spinal column injury include falls, animal attacks and gunshot wounds. Spinal fractures can also result from non-traumatic causes, such as neoplasia, infection and metabolic bone disease.
About Primary and Secondary Spinal Cord Injuries
 Spinal cord injury is divided into two categories: primary injury and secondary injury. Primary injury includes mechanical damage such as concussion, compression, shearing, laceration and elongation.
Spinal cord injury is divided into two categories: primary injury and secondary injury. Primary injury includes mechanical damage such as concussion, compression, shearing, laceration and elongation.
Primary injury causes tissue damage that begins a cascade of neurotoxicity known as secondary injury. When neurons are damaged by hemorrhage, ischemia and edema caused by the primary injury, neurotoxic substances are released, including free radicals, excitatory neurotransmitters, cytokines and other inflammatory mediators, which cause further neuronal injury and death.
Treatment of spinal fractures and luxation/subluxation is aimed at stopping further mechanical damage through spinal stabilization, and providing supportive care such as anti-inflammatories and fluids to treat the secondary injury by providing adequate perfusion and oxygenation of the spinal cord.
Evaluating and Stabilizing Concurrent and Life-Threatening Injuries
Patients should be initially evaluated and stabilized for concurrent and life-threatening injuries. Up to 83% of patients with vertebral column trauma have concurrent injuries.
Determining if a vertebral column injury requires stabilization is based on the “three-compartment model.” The vertebral column is divided into dorsal, middle and ventral compartments:
- The dorsal compartment includes the area of the vertebra from the spinous process up to the floor of the canal.
- The middle compartment includes the dorsal longitudinal ligament, dorsal annulus fibrosus and dorsal aspect of the vertebral body (basically the floor of the canal).
- The ventral compartment is the remainder of the vertebral body and disc.
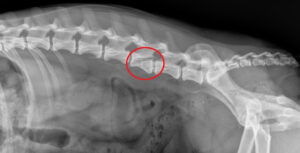
Advanced imaging is required to fully evaluate the stability of all compartments of the vertebral column. 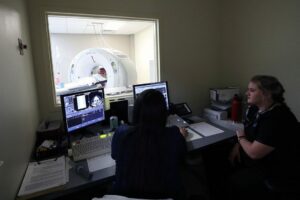 Radiographs are helpful in initial screening of vertebral column injuries and the entire spine should be evaluated to rule out multiple sites of injury. However, radiographs underestimate the degree of injury to the middle and dorsal compartments.
Radiographs are helpful in initial screening of vertebral column injuries and the entire spine should be evaluated to rule out multiple sites of injury. However, radiographs underestimate the degree of injury to the middle and dorsal compartments.
CT is the best modality for evaluating spinal fractures and provides better resolution of the dorsal and middle compartments. MRI is the best modality for evaluating the spinal cord parenchyma and to detect hemorrhage, edema and intervertebral disc herniation.
Treatment for Vertebral Column Injuries
Treatment of vertebral column injuries is focused on stopping additional primary injury caused by instability and spinal cord compression, along with limiting secondary injury by maintaining cardiovascular support to decrease hypoxia and ischemia, and improve perfusion of the spinal cord.
Corticosteroid use is controversial in spinal cord injury, with no proven benefit of methylprednisolone, or high dose dexamethasone. The decision to treat vertebral column injury is made on an individual case basis because no randomized, controlled studies have compared surgical to nonsurgical management.
Nonsurgical management is recommended in patients with minimal neurologic deficits, stable fractures and lack of concurrent injuries. Treatment consists of cage rest and potentially external coaptation. However, malpositioned or displaced bandages can worsen vertebral fractures.
Surgical management is recommended for intractable pain, worsening neurologic deficits and unstable fractures. Many methods of surgical fixation are available, including but not limited to, pins and PMMA, locking plates and external skeletal fixation.
Prognosis for Spinal Cord Trauma
Prognosis for vertebral column injuries is based on neurologic status. Patients that have absent nociception have a 5% chance of regaining ambulation, but still may not regain nociception or continence.
Due to this poor prognosis, many patients are euthanized. On the other hand, prognosis in patients with nociception is good. Between 80-100% of patients treated medically or surgically will regain function.


