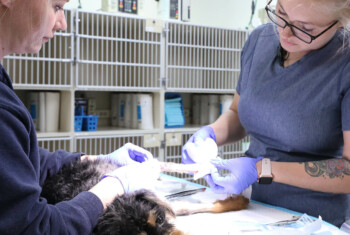
Successfully Managing Pet Glucose Levels
Even the most astute owner finds it difficult to predict what their pet’s blood glucose is.
Historically, the goal of diabetic treatment was to simply establish and maintain glycemic control, based largely on owner observation of clinical signs. Feline diabetics were thought to be insulin sensitive and a challenge to regulate. In the dog, it was accepted that diabetic cataracts would develop with blindness occurring in ~12 months. As veterinarians, we strive to provide our companion animals with the best quality of life possible and observation is key.
Advancements in Insulin Application
Even the most astute owner finds it difficult to predict what their pet’s blood glucose is. Feeling weak or lethargic is just not something a pet can easily communicate. When clinical signs of hypoglycemia or hyperglycemia develop, the blood glucose is usually dangerously high or life-threateningly low.
Historically, our goals in the management of diabetes in dogs and cats have been to control the patient’s clinical signs (PU/PD/PF) and to avoid diabetic ketoacidosis. Recent innovations in the combined use of longer-acting insulin, easy-to-use home blood glucose monitors, and diet options – low-carbohydrate diets for cats and low glycemic index carbohydrate options for dogs – are redefining the standard of care.
Exogenous insulin is the mainstay of treatment of canine and feline diabetes. Diabetes has quickly become a significant part of our collective mainstream consciousness with the current epidemic. The idea of home blood glucose monitoring (HBGM) has become familiar to most. It shouldn’t come as a surprise that owner-initiated HBGM is common.
What we, as veterinary professionals, should strive to understand and embrace is the progressive trend of veterinarian-initiated HBGM. A HBGM protocol should be instituted by the veterinarian, not by the pet owner.
Insulin administration in the face of hypoglycemia carries significant morbidity and mortality. One of the most important reasons for HBGM in patients with diabetes is the dynamic nature of the disease: with all other variables kept constant, blood glucose values in the diabetic patient vary significantly on a day-by-day and hour-by-hour basis. This same variability documented in human diabetics also occurs in dogs and cats.
Known Glucose Level Variables
Variables known to influence glucose include stress, excitement, exercise, quality and quantity of diet, and amount of insulin absorbed. Varying the injection site leads to different absorption and is not advised.
Variability in glucose also occurs in the absence of an explainable cause. Inconsistent glucose values are a source of frustration. After daily HBGM is instituted, the magnitude of the fluctuations becomes apparent. Simply stated, every day is not the same. In the absence of HBGM, one is unlikely to be aware of the inconsistent values, as dogs and cats are quite tolerant to both hypo- and hyperglycemia, with a paucity of recognizable signs.
Glucose levels in real time
Knowing what the glucose is in real time is empowering, as it allows the pet owner to take an active role in the management of their pet’s diabetes and gives the veterinarian data to make educated insulin dosing decisions.
What is Fructosamine?
Fructosamine levels are a valuable measure of the average blood glucose for the previous 3 weeks, but do not reflect daily fluctuations. Real-time values allow for real-time decision-making. None of us would give our own diabetic pet, or instruct an owner, to give insulin in the face of hypoglycemia.
Unfortunately, this frequently happens because of lack of HBGM. Likewise, if the glucose was high in the face of emerging disease, dietary indiscretion, stress, excitement or a Somogyi phenomenon (insulin-induced hypoglycemia, followed by rebound hyperglycemia), a blood glucose curve (BGC) or monitoring four times daily can be implemented to determine the correct insulin dosage.
What to diagnose?
As a profession, we have tended to err towards hyperglycemia over hypoglycemia, due to the negative ramifications of hypoglycemia. Long-term complications associated with hyperglycemia, can significantly impact a patient’s quality of life including diabetic neuropathy, and diabetic cataracts in dogs. Patients who have their glucose monitored at home are generally on higher dosages of insulin safely, with better glycemic control. Diabetic remission in the cat is much more likely with tight glycemic control.
Letting Owners Take Control
Guidelines for the Management of Diabetes published in the May/June 2010 AAHA Journal advised HBGM. HBGM eliminates the stress of transport and the hospital environment and allows generation of a 12-14 hour BGC. At home, the BGC is not truncated by hospital hours, and the pet’s daily routine relative to exercise and feeding are followed.
The key difference here is who collects the data. Empowering the owner to measure glucose at home ensures accurate and complete data and allows the clinician to adjust the insulin dose. Owners are asked to perform a BGC for review when rechecked. According to the AAHA article, owner compliance with long-term HBGM is excellent and does not impact recheck.
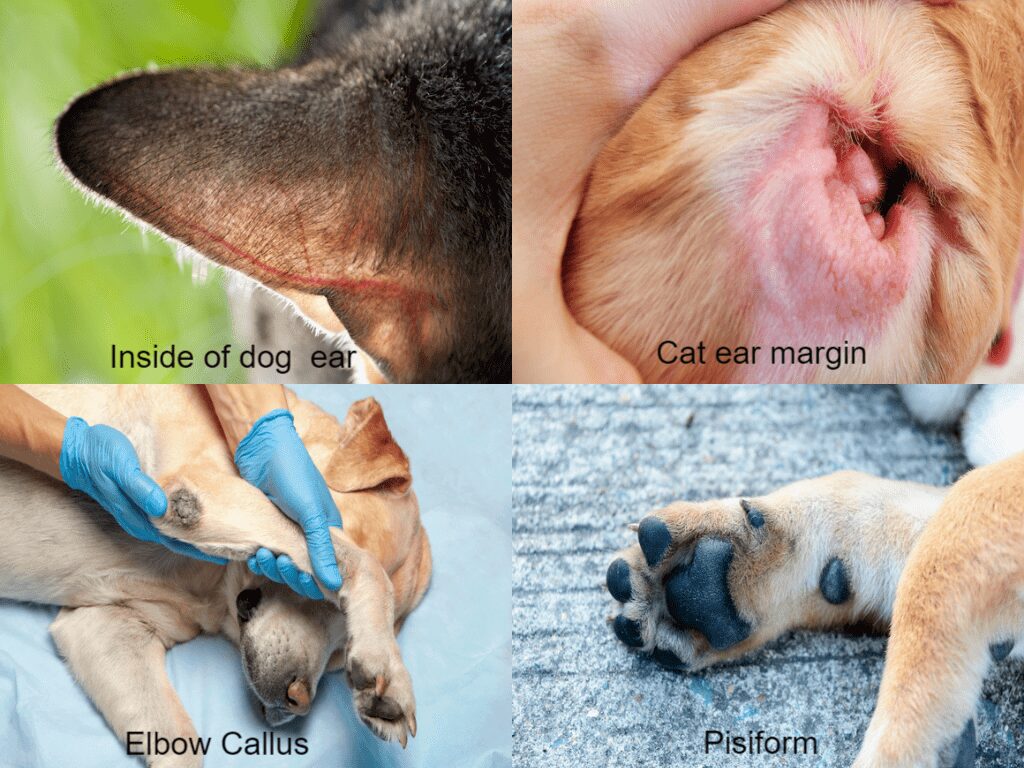
Most owners are able to learn how to collect capillary blood for HBGM, and most pets tolerate the procedure. Preferred testing sites in the cat and dog are the pisiform pad, or non-weight-bearing paw pad proximal to the carpal pad on the forelimbs, (Figure 1) and the lateral ear vein (Figure 2).
The outer pinna is best in the cat, while the inner pinna is best in the dog, especially in dogs with floppy ears (Figure 3). The buccal mucosa is optimal in larger dogs with good temperament. The lateral elbow callus in dogs makes sampling easy when present (Figure 4). Small dogs, or those who exhibit a biting tendency when their ears, feet or mouth are handled, do best with testing the redundant skin fold at the dorsal tail base (Figure 5), where a small area of hair can be clipped to facilitate testing.
Blood glucose is ideally measured in the morning, prior to food and insulin, and 12 hours later in the evening. The therapeutic goals are patient- and owner-driven, but, in general, the glucose should not be higher than 300 or lower than 80 mg/dl.
HBGM puts these seemingly lofty goals within reach, thereby improving quality of life for pet and owner. HBGM can be simply and safely mastered by most owners, which will result in a longer and healthier life for their pets, and a more satisfied owner and veterinarian.